- About
Our consultants
Meet our experienced team of consultantsSupport team
Meet our support team working alongside our doctors to deliver the very best careOur clinic
Discover more about The Fertility & Gynaecology Academy
- Patient journey
I am a...
Learn about the services relevant to your fertility journeyThe journey...
Learn about what's involved in fertility treatment
- Fertility tests
Packages
Fertility testing packages to take the hassle out of investigations
More screening options
Find out about our additional screening options - Treatments
Getting pregnant
Fertility treatments to help you achieve your dream
Add-on treatments
Learn about add-on fertility treatments
Supporting treatments
Additional services to support you on your fertility journey - Success rates
- Knowledge hub
Watch, read, and learn
Expand your knowledge on all aspects of fertilityLatest article
- Pricing
Financing fertility treatment
Honest and transparent pricing for peace of mind
No two patients have the exact same treatment but here we have provided an example patient journey to help illustrate what a straight-forward IVF cycle might look like cost-wise.
- Contact
IVF / ICSI
We have a wealth of experience of using IVF and ICSI successfully to help couples achieve conception.
We have consistently achieved impressive results, which you can see from our recent success rates.
We have a wealth of experience of using IVF and ICSI successfully to help couples achieve conception.
We have consistently achieved impressive results, which you can see from our recent success rates.
Two of the most widely known treatments for male and female infertility are In-Vitro Fertilisation (IVF) and Intracytoplasmic Sperm Injection (ICSI).


In-Vitro Fertilisation (IVF)
In-Vitro Fertilisation (IVF) is a procedure that involves surgical removal of an egg from the woman’s ovaries and fertilising it with sperm in the laboratory. The fertilised egg or embryo is then placed back into the woman’s womb to grow and develop.
- Originally designed for treatment of women with blocked Fallopian tubes.
- Endometriosis and pelvic adhesions.
- Ovulatory disorders.
- Suboptimal sperm parameters.
- Unexplained infertility.
You normally produce one egg in a cycle. As not every egg fertilises and not every embryo progresses to implant, we aim to make you produce a reasonable number of eggs (8-12) through “Controlled Ovarian Stimulation”.
Through different protocols tailored to individual patients’ needs we prepare you for the IVF cycle using two types of drugs; one to stimulate your ovaries to produce eggs (FSH ± HMG injections) and the other to stop your pituitary gland from controlling your ovaries so that you do not ovulate before the time for egg collection.
Before you start the stimulatory injections you will have a scan and blood test to make sure that you have a good starting point. You will have another blood test and possibly a scan 3-4 days later to assess the response of your ovaries. You will then have a blood test and a scan every other day to fine tune your response. On average it takes 10-12 days of injections until the eggs are ready. Once the eggs are ready we give you a late night trigger injection to mature the eggs. The egg collection will take place about 36 hours later.
Eggs are collected under ultrasound guidance with a needle going through the vagina into the follicles to retrieve the eggs. You will not feel it as you will have intravenous sedation. You should not eat or drink anything from midnight before your procedure. Once the eggs are recovered, you will be transferred to the recovery room and will usually be ready to leave one or two hours later. However, it is important to have somebody to accompany you. You should not drive a car for 24 hours. You will need to start progesterone in the form of suppositories or deep intramuscular injection from the night after the egg collection.
It is common to feel some bloating and have some lower abdominal discomfort for a couple of days. You need to drink fluids and take paracetamol tablets if you feel you need them. A small amount of vaginal bleeding is normal and it is preferable to use sanitary pads rather than tampons.
We prefer that male partners produce their semen sample at the clinic. In extreme circumstances, it may be possible for men to produce at home or in a hotel but it is essential that you discuss this with your consultant. You need to abstain from sex for 2-3 days (but not more than 5) prior to the day of egg collection.
The eggs are taken to the laboratory and, a few hours later are inseminated with your prepared semen sample. About 18 hours later, they are examined for fertilisation and then after 24 hours for division (cleavage). If cleaved embryos have developed, embryo transfer proceeds.
Sadly, sometimes no eggs fertilise, either because the eggs are of poor quality, or because of an unsuspected semen factor, or – rarely – for reasons that cannot be explained. If fertilisation does not occur it is disappointing but IVF can be performed again. Usually, for a subsequent attempt we recommend ICSI.
This is normally carried out 2-5 days after the egg collection. If you have a reasonable number of good quality embryos by day three you might be advised to have the embryo transfer on day 5 (blastocyst transfer). A fine tube or catheter is passed through the cervix and the embryos are injected in a minute amount of culture medium. It does not usually need sedation. Most patients need a full bladder to make the delicate procedure of ET easier. You need to drink a litre of fluid an hour prior to your ET.
We can transfer a maximum of two embryos according to the HFEA code of practice except if you are above forty years old and using your own eggs. In this instance we can replace three (day 2 or day 3) embryos.
If the surplus embryos after the transfer are of good quality they will be frozen and stored in liquid nitrogen. Embryos may be stored, if both partners give consent, for up to 10 years normally. You must remain in contact with the Clinic as you are completely responsible for confirming that you wish the embryos to remain in storage. You are responsible for paying an annual fee to cover administration and storage. You must also inform The Fertility and Gynaecology Academy of any change of address or personal circumstances. Failure to establish any contact will result in the embryos being discarded at the end of the consented storage period, as required under the HFEA Act 1990.
Prior to replacement, frozen embryos are thawed when the womb lining is ready. Not all embryos survive the freeze/thaw procedure and the chance of pregnancy might be reduced when using frozen embryos when compared to fresh embryos.
It is wise to rest after the egg collection and you might need to take the following day off work. It is important to try to relax and take things easy after the embryo transfer until implantation takes place (a week after egg collection) – preferably until you have your pregnancy test (14 days after egg collection). The embryos are safe in your womb and although you can walk, shower and undertake your normal daily activities, it is best to avoid strenuous activity and heavy lifting. Although sexual intercourse is not prohibited most couples prefer to avoid sex until the pregnancy test.
IVF cycles starting from just £3,750
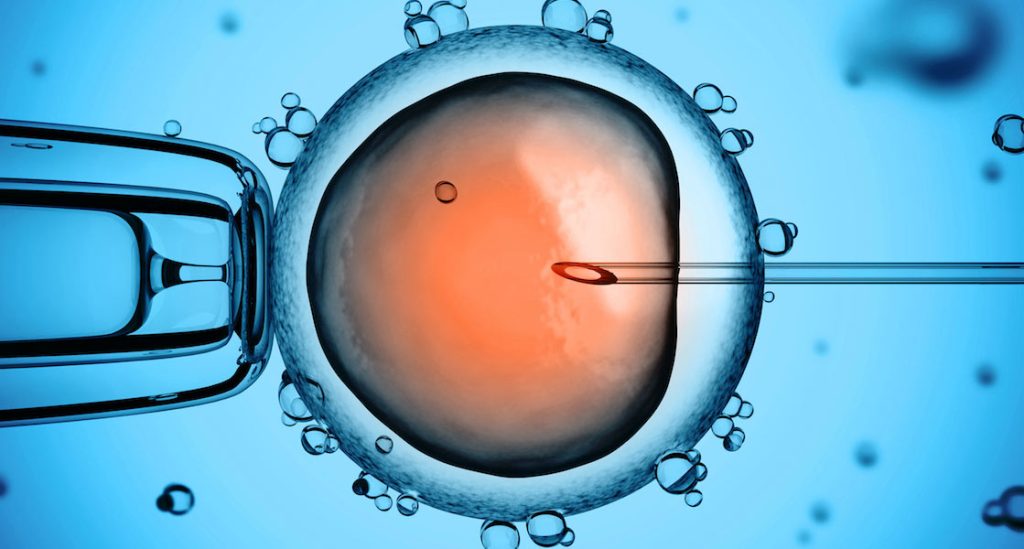
Intracytoplasmic Sperm Injection (ICSI)
ICSI is a technique to fertilise an egg by micro-injecting sperm that would otherwise not be able to achieve fertilisation. The fertilisation rate through ICSI per egg is about 60-70%.
The female partner undergoes the same preparation and egg collection as in conventional IVF. The only difference is in the fertilisation process in the IVF laboratory. A few hours after the egg collection, only mature eggs are injected with sperm under the microscope and checked for fertilisation the following morning.
- Very low sperm count, motility or forward progressive motility.
- High percentage of abnormal sperm forms.
- High levels of anti-sperm antibodies in the semen.
- Surgically retrieved sperm from the epididymis (PESA) or testis (TESA).
- History of poor fertilisation (less than 30%) in a previous IVF cycle.
- When there is doubt about fertilisation. For example: unexplained infertility – we may split the eggs between IVF and ICSI to avoid the disappointment of failure.
Inheritance Of Cystic Fibrosis (CF) Gene: Some men have no sperm in the ejaculate because the vas deferens, the tubes that carry spermatozoa from the testes to the penis, is absent; a condition called Congenital Bilateral Absence of the Vas Deferens (CBAVD). Such men are also more likely to carry the cystic fibrosis gene. You can be a carrier of cystic fibrosis without congenital absence of the vas deferens since about 1 in 25 in the Northern European population is a carrier of that gene. If you have congenital absence of the vas deferens we recommend that you have the test for the cystic fibrosis gene. If you are a carrier your partner would need to be checked too.
Deletions On The Y Chromosome: Some men with very few spermatozoa in their ejaculate have an abnormality with their Y chromosome. This means that a son born to a man who carries such a problem may also have a damaged Y chromosome. We recommend chromosome testing to see if a sub-fertile man carries this minor abnormality. Most couples having ICSI prefer to use their own sperm rather than donor semen, which is the only other alternative.
Congenital Abnormalities: It is natural for any parent to worry that there may be something wrong with their child. Without treatment, the risk of a child with a congenital abnormality is around 2 to 2.5%. Some researchers have suggested that the risk of a problem following ICSI is the same as in IVF or in women conceiving without treatment.


IVF & ICSI success rates
Success rates vary depending on the type of problem and the factors personal to individual women. These include the age of the woman being treated, her ovarian reserve, the number of eggs she produces, the quality of the sperm, the number of embryos that result, and the number of embryos transferred.
Get in touch today
If you are considering IVF or ICSI and have any questions, please call us on 020 7224 1880.
Alternatively, if you’re ready to go ahead, you can book a consultation by clicking below.


